Yes, you can get Type 1 diabetes as an adult. My husband’s diagnosis at age 33 had a huge effect on our family, but with a positive attitude and a lot of trial and error, you can find your new normal and live life to the fullest!

Hi friends!
As many of you know if you follow me on social media, two weeks ago my husband was diagnosed with Type 1 diabetes at the age of 33. Since this is a major diagnosis, impacting pretty much all areas of our life, I wanted to take some time and write down our story. I’ve discovered that many people don’t actually know a lot about type 1 diabetes so I think it’s a good opportunity to use this platform to educate. I’ve also realized just how much a diagnosis like this (of a chronic, long-term autoimmune disease) affects not only the person themselves, but family members and those around them as well….so I wanted to give you some insight into how it’s affecting him, me and our family in general.

Types of Diabetes
So, first a little clarification for those of you who don’t know -there are several types of diabetes. Before his diagnosis, I knew the basics about type 1 and 2 and that was about it. I was not an expert then and I’m certainly not an expert now, but I’ve done a lot of reading lately and learned a lot! So here’s a brief overview:
Type 1 diabetes is an autoimmune disease with a fairly sudden onset. While it is most often known for being diagnosed in young children and teens (often known as juvenile diabetes), it’s actually almost as common for people in their 20’s & 30’s (and beyond) to be diagnosed. With Type 1, the body’s immune system attacks the cells in the pancreas that produce insulin so they stop producing it. While the exact cause is unknown, it’s likely a combination of genes you’re born with and an environmental trigger that activates it. If you’re not producing insulin, sugar builds up in the blood instead of going into cells where it’s needed…so you need injected insulin (a combination of long-acting and short-acting) for the rest of your life.
Type 2 diabetes has a more gradual onset. Your body is still producing insulin, you just become less sensitive to it over time. Typically, you can initially manage Type 2 with diet and exercise and take oral medication to stimulate the pancreas to make more insulin. Eventually, your pancreas may stop working and you’ll require insulin. The cause of type 2 diabetes is multifactorial- you can inherit genes that make you more susceptible but lifestyle factors like diet, exercise & obesity also play a role.
In addition, there’s another type known as LADA- latent autoimmune diabetes in adults (sometimes called type 1.5 diabetes), that is often initially misdiagnosed as Type 2. They have similar symptoms but LADA develops faster and people are often at a healthy weight, whereas Type 2 is often (but not always) diagnosed in people who are overweight. So even though they may initially be able to get by because their pancreas is still producing some insulin, oral drugs prescribed for type 2, like metformin, will eventually stop working for LADA patients because their immune system will continue to destroy insulin-producing cells.
There are blood tests that can be used to diagnose LADA by measuring the amount of c-peptides in the blood. C-peptides are a byproduct of insulin production, so low levels can indicate that your body is not producing much insulin on its own. Another blood test often given to LADA patients looks for the presence of insulin-destroying antibodies.
Hubby’s Story
Here’s what happened to my husband: Starting sometime around the beginning of 2018, we noticed he was having some unusual symptoms that included increased thirst, increased hunger and increased urination. He was feeling generally sluggish, having some vision changes, losing some weight etc. I prompted him several times to go to the doctor for his annual exam. We knew something was wrong but weren’t sure whether it was diabetes, thyroid-related etc.
He finally scheduled his exam for the first week of March and on Friday, March 9th he had his appointment where he shared everything with his doctor. They took a lot of blood for bloodwork and also took a urine sample. Within an hour or two, they had called him back and told him that his urine test showed his blood sugar was over 400, there were ketones in his urine and he needed to go to the ER immediately.
His parents came over to watch the kids and we headed to the ER. There, they did more bloodwork, gave him insulin and fluid and decided to admit him. My parents drove from Chicago to stay with the kids while we handled all of this.
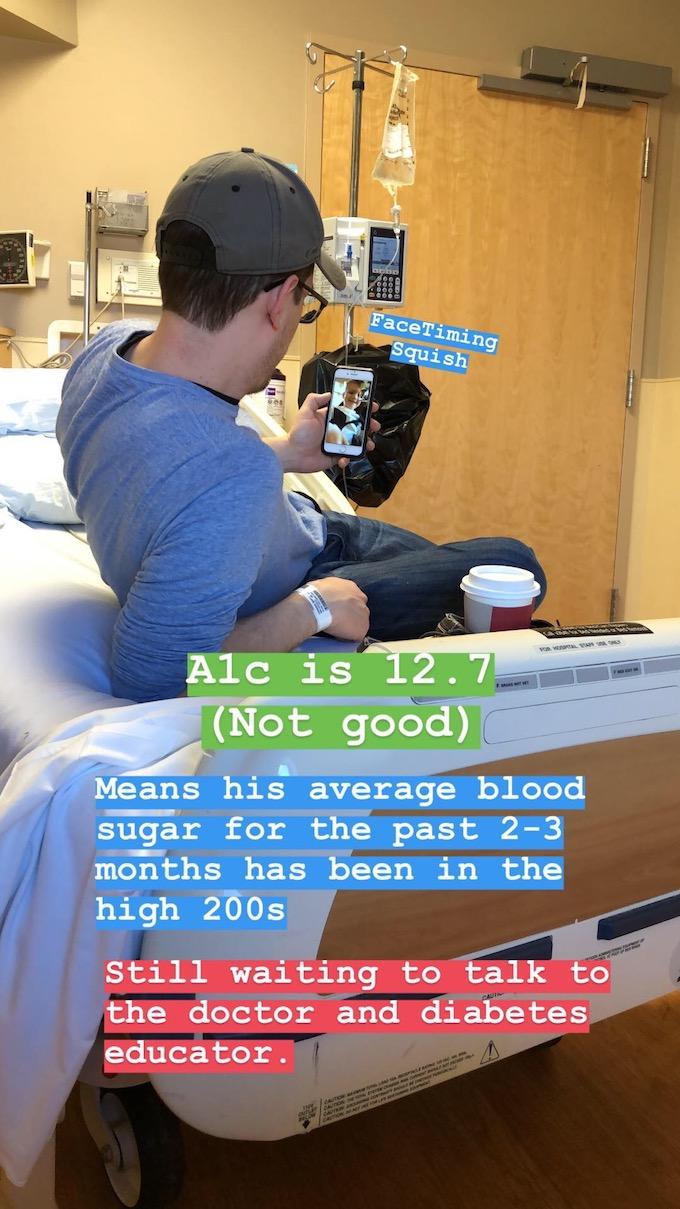
Saturday morning he was officially diagnosed with Type 1 diabetes. We got the results of his Hemoglobin A1c blood test back and it was 12.7, which is extremely high. A1c is a test used to measure a person’s average blood glucose level over the past 2-3 months. Normal is below 5.7. So, his results indicated that his average blood sugar over the past 3 months was in the high 200’s. Normal blood sugar levels are 70-99 when fasting and below 140 within 2 hours after eating.
They decided to keep him at the hospital one more night so that they could continue to track his blood sugar and see how it was responding to the insulin. We were also supposed to speak to a diabetes educator but apparently, at the hospital we were at, they don’t work on the weekends. So, since we were there Friday night to Sunday afternoon, we didn’t speak to one.

However, he had an awesome nurse that really stepped up to help teach us about some of his new daily activities like checking his blood sugar and injecting insulin and let him practice on himself so he was comfortable doing it.
Sunday afternoon we were sent home with instructions to check his sugar at least 4 times a day and see an endocrinologist within 3 days. We were completely overwhelmed but trying to just take things one day at a time. On the way home, we stopped at the pharmacy to pick up all the supplies including a glucose monitor, test strips, lancets, alcohol swabs, insulin pens and more.
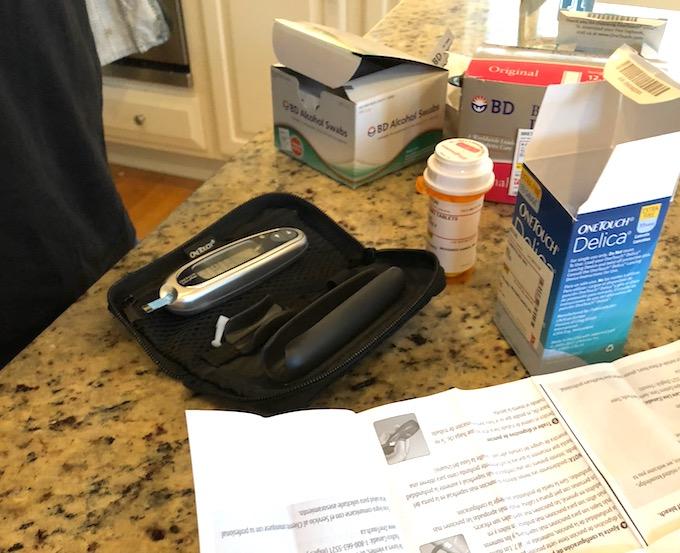
The first time we had to do everything at home was incredibly stressful. Both the glucose monitor and the insulin pens were slightly different than the ones he’d been practicing with at the hospital. The glucose monitor was different. The insulin pens he had practiced on had a type of safety cap so only the very tip of the needle came out wheras the kind we came home with had the whole needle exposed. At the hospital they threw away the insulin pens after injecting him, wheras the ones we came home with you just throw away the needle and the pen itself has enough insulin in it for many injections.
We tried to make an appointment with an endocrinologist, found out we needed a referral, got a referral and still haven’t even been able to get an appointment on the calendar (two weeks later). Our hope is to get him on both a continuous glucose monitor and an insulin pump as soon as possible, we’re just not sure exactly how soon that will be.

Luckily my husband was able to take a few days off work to take some time and adjust to everything. We experienced our first low blood sugar episode and now have stashes of fruit snacks and juice boxes all around the house, in both cars, in my purse, out in the garage gym, at work, next to the bed etc.
We definitely would not have survived the first few days without my online community. My friend Mary Ellen (who is an RD and Type 1 diabetic herself) has been endlessly patient and answered dozens of texts from me each day as new questions and situations came up that we had no clue how to handle. We also had several certified diabetes educators who follow me on social media reach out and be willing to answer questions for us.
I may be a Registered Dietitian, but that does not automatically make me a diabetes expert. So I am learning right along with him.
We ordered a few books that people recommended (Think Like A Pancreas and Sugar Surfing) and also went back to see our family doctor to answer some immediate questions, as well as get prescriptions for new supplies as we discovered that the needles that came with the insulin pens he got were a bit too long for him. You’re supposed to pinch your skin and inject the insulin, without pushing it into the muscle. Since he doesn’t have a ton of body fat, sometimes it’s tricky to keep a longer needle from going in too far. We also discovered the finger-sticking needles he got were too fine and not making his fingers bleed enough to get a sample to test his blood sugar.
We’ve been testing his blood sugar about 6 times a day and are using an app to keep track of all the readings so we can analyze them and share with doctors. We have learned how to count carbs, looked up the carb counts of a lot of foods, learned how to dose insulin and treat highs and lows and more….all in the span of just a few days.

So Many Questions
You never really think about just how many questions and unknowns come along with a diagnosis like this until it actually happens and you find yourself with a mile long list of questions. Here are just some of the things that came up:
- Can he take his long acting and short acting insulin at the same time in the morning?
- What should his daily carb goal be?
- Should he be taking insulin to correct his blood sugar levels before meals as well as in anticipation of what he’s about to eat?
- How many grams of carbs does he need to correct a low?
- How will he know when his blood sugar gets too low?
- What if we’re going out to eat and don’t know how long it will be until we eat? Does he need to take all the supplies with him to the restaurant?
- What do we do the first time he gets sick and doesn’t feel like eating? Or if he takes insulin and then throws up?
- How should he handle drinking alcohol?
- Should he be taking insulin before bed even if he’s not having a snack? What should he be eating for a bedtime snack?
- What should he do about exercising? Eat beforehand? Take insulin? Not take insulin? Can he exercise when his sugar is high?
- How soon can we get a pump and a CGM?
- Are our kids going to get Type 1?
- What do we do if we go on vacation and he loses his insulin?
These are just a few of the questions we had to work through after his diagnosis. And I still have a running list of questions for when we finally get in to see the endocrinologist.

A Family Affair
This diagnosis is obviously having a huge impact on my husband. We’re in for a lifelong series of expenses and constant adjustments. It’s his body and he’s the only one who truly knows how he’s feeling. He has to be responsible about checking his sugar levels and taking insulin. He has to pay attention to how certain foods make him feel, what causes his sugar to spike and drop, etc. He has to prick his finger and inject himself constantly until we’re able to get him on a pump and get him a continuous glucose monitor.
There will constantly be new experiences that he has to learn how they will affect his body (lifting, cardio, yardwork in the summer, playing with the kids, not getting enough sleep etc). He has to remember to bring his supplies with him to work so he has his insulin in case he gets stuck at work and can’t come home for lunch, or in case he goes low during a meeting at work and needs to raise his blood sugar. It’s way harder to eat out if he doesn’t know the exact carb counts for what’s on the menu. (Not impossible…just takes more planning)

Right now our kids are fairly unaware of what’s going on but Squish does see him checking his sugar and giving shots and asks questions about it so we’re trying to find ways to explain it to him in a way his three-year-old mind can understand. As they get older, we’ll have to teach them what signs to look for when daddy has low blood sugar and what to do to help him (ie how to call 911, where his food supplies are, etc). We’re also dealing with the fact that the fruit snacks and juice boxes we have on hand for daddy are some of Squish’s favorite snacks…so we have to keep him out of those.
As for how it’s affecting me? It is…in a huge way. I’m constantly worried about him, want to know what his blood sugar is all the time, am always afraid it’s going to go low while he’s driving, or in the middle of the night while he’s sleeping (one of the main reasons why we want to get him on a CGM as soon as possible…because you can set alerts to go off if it goes too high or too low and i’ll be able to see his blood sugar levels through an app on my phone).
I’m worried about complications that could arise in the future and whether our kids are going to get this same diagnosis. I’ve had to learn how to use the glucose monitor to check his sugar, how to inject insulin so he can rotate injection sites to different parts of his body that he can’t reach by himself (like his tricep).

I’ve had to make a lot of adjustments to the way I cook. No longer can I just throw whatever I feel like in a pan. He needs to know how many carbs he’s eating so I have to do a lot of measuring. I made a stuffed pepper bake the other day and I measured all the ingredients, looked up the carb counts for all of them, divided the dish into 4 servings etc so he’d know exactly how many carbs were in each portion. Same thing with the salmon burgers I made for dinner last night. I haven’t exactly figured out yet how to tackle things like soups and casseroles where there’s so much stuff all mixed together making it harder to measure what’s in each portion but I’m sure that will come with time and practice and probably using something like My Fitness Pal.
While hubby doesn’t need to follow a crazy low-carb diet, he does have to be smarter about the carbs he’s eating. No more snacking willy-nilly on things like chips and pretzels…instead, he’s focusing more on getting his carbs from things like fruits, vegetables and whole grains. It’s not a huge change from the way he was eating before but there have definitely been some adjustments.
Some people have asked if that means I’m eating low carb..and the answer is no not really…I’m still snacking on chips with hummus while drinking a beer and eating a handful of m&ms before bed…but I’m definitely more aware. And I do occasionally feel guilty when I’m eating a carb-heavy snack like that that I know isn’t the best choice for him.
Similarly, I’m affected by things like the fact that we probably won’t be ordering a basket of chips and salsa when we go out to eat at a Mexican restaurant anymore..because I’d be eating them by myself. Or the fact that I probably won’t bake my standard cookies as often anymore because he won’t be eating them as frequently and I don’t want them to be around to tempt him. Again, it’s not like he can’t have sweets…but before, he could come home from work and grab a cookie and it was no big deal. Now he needs to know exactly how many carbs are in that cookie, factor that into the amount of insulin he’s taking etc.

I’m trying to observe him closely and learn how his moods change as his blood sugar changes. We know that when it’s super high or super low, he gets increasingly irritable and anxious (not his fault) so during those times I’m trying to manage the kids and keep them calm and out of his way while he works on regulating his sugar.
I’m trying to plan ahead, make sure we know what we’re doing and where we’re going whenever we leave the house so we know what supplies to take, whether he needs to eat beforehand, pack a snack etc. We can’t even just leave on a spur of the moment family walk anymore without making sure we have some fruit snacks or a juice box to take with us in case his blood sugar goes low.
I’m sure reading through all this may sound like I’m complaining…but I’m not. I’m just sharing our experience and give people an overall picture of what it’s like to go through a diagnosis like this. It’s overwhelming and scary and definitely impacts everyone in the family and all aspects of your life together.

The good news is, we make a great team. We’re both smart people and are willing to work hard together to figure things out, get our questions answered and experiment with various things to figure out what works best. We were already eating healthy and exercising so although I’ve had to make some adjustments in the kitchen, they’ve been fairly minor and overall, our lifestyles changes have been relatively minor and more adaptive versus a major diet and exercise overhaul.
The medication side has definitely been the most challenging for us. We’re still making changes and trying to figure out what works best to keep his blood sugar under control and we know there’s no instant fix. So far we’ve had to increase his dose of long-acting insulin, change his correction factor (carbs per unit insulin) and split his long-acting insulin in half to take it twice a day instead of just once because it was wearing off too quickly and causing his sugar to get way too high in the morning. We also learned that working out when his sugar was already high makes his sugar spike even higher, whereas if it’s normal, working out can make it drop. Almost all the stuff we’re doing with the insulin has been based on our own research and with the help of Mary Ellen who has been invaluable in sharing both her clinical knowledge of diabetes and her first-hand experiences.
I’m sure there will be good days and bad days from here on out but we’ll face them together and do what we can to make the best of our new normal – life with Type 1 Diabetes. I’m forever grateful that my hubby is so level-headed and is facing this diagnosis with a positive attitude. He’s already conquered so many aspects of the disease and is willing to do whatever it takes to stay as healthy as possible for the future.

Thanks for letting me share our story! If you have any questions that I didn’t already answer, feel free to send them our way!
Enjoy!
–Lindsay–
LEARN HOW FOOD AFFECTS YOUR BODY.
Get my free Table Talk email series where I share bite-sized nutrition information about carbs, protein, and fat, plus bonus information about snacks and sugar!



Thank you for sharing your story. I admire your openness and candor while going through this period of great change. Wishing you and your family the very best. And please know nor once did I ever view what you wrote as complaining. This diagnosis have totally altered your sense of normal and you are getting acquainted with your new normal. Your post was about just that.
Thank you very much! We appreciate it!
Of course!!!!! My best to you guys!!!!
I was diagnosed type 2 15 years ago and recently became type 1. Something I learned from a diabetic nutritionist is to take short acting insulin 10-15 minutes before eating. I carry a small bag with me at all times with glucose tablets, monitor and insulin. I use the app CalorieKing for carb counts and take amount of carbs divided by 7 and that is the amount of insulin I take before a meal. I have experienced occasional lows and find orange juice or small soda follow d by a protein (peanut butter) gets it up and prevents another drop. Good luck!
Yes, what a HUGE life adjustment. It will eventually become the new normal. Some things that helped calm my nerves when my husband was diagnosed and also in regard to a good friend that’s been type 1 since childhood – tell everyone the symptoms to watch for in regard to low blood sugar. My first wrong impression was “certainly they can tell that their sugar is too low.” That is not necessarily the case….at all! But having friends and colleagues know the symptoms and how to treat was calming. Also, dogs are SO aware. We had a dog, a small one, that slept with us. He was not trained to detect low blood sugar, he was my husband’s best friend. In the middle of the night, the dog started acting weird. He tried to wake my husband. When my husband didn’t respond, he woke me. Not in a “I have to go out” way, but in a way like “something is not right with my dad.” My husband’s sugar levels were alarmingly low and the dr confirmed that had we not woken up and treated it, he most likely would have ended up……….
Please don’t be alarmed by this, but really tune into your “6th sense”, whether that be instinct, the little voice in your head, an animal, etc.
yep! i made sure to have him tell his coworkers what to look for at work! Animals are so cool!
Wishing your and your family the best in figuring all this out. My Son was diagnosed 10 years ago as Type one Diabetic with an A1C of 18. The highest his doctor had ever seen. It has taken many years of trial and era for us to feel like we have a good understanding of this disease. My son has had many complications from this but we are now at a good spot with feeling like we have a hold on things. He has just gotten and insulin pump and a CGM in the last 6 months, what a difference it has made for him. It’s all about educating yourself and perseverance. It sounds like you both are on the right track with that. It truly takes a team as it can feel overwhelming at times. Hang in there and hoping you find the answers you are seeking.
i agree! definitely overwhelming but manageable. Glad the pump and CGM are helping your son!!
Thank you for sharing Lindsay. Hooray for animals, they are the greatest! Maybe your cat can learn to detect low blood sugar. I’m sure this will be a life long adjustment because you will always be learning new things. But I know you will manage very well. Looking forward to some low carb recipes too.
Thanks Carol!
Checkout Mastering Diabetes online, they are running a summit of many experts soon
They are both type 1 diabetics for many years.
I am a type 2 Diabetic. I empathize with your diagnosis. Kathleen
I’ve seen stuff about that. will check it out. thanks!
Reading your story just gives me major flashbacks. You are absolutely right that it is not just a change in his life but the entire family. My kids are always asking what my blood sugar number is when I check. It is important to teach them as well no matter how young they may be. Thanks for sharing your story. We are so lucky that we were diagnosed at a time where technology is on our side. Between the insulin pump and the CGM I just recently got it makes managing this disease just a little bit easier. The body still does what it wants and sometimes what you did yesterday doesn’t work today. That is a very frustrating part. The moment you think you figured it out your body reacts differently. Keep on sharing what you have learned!
Will do! Thanks for all your help so far.
I can’t fully relate since Type I is very different from gestational diabetes, which I had when I was pregnant, but you mentioned eating out, so I wanted to provide a small tip. I would suggest not being afraid to ask the restaurant to make modifications. I often substituted whole wheat sandwich bread for hamburger buns, veggies such as broccoli for white rice, etc. Since my pregnancy I have given up sugar and recently tested negative for pre-diabetes. I am almost grateful that I had that wake-up call because it showed me how challenging life as a diabetic can be with testing your numbers multiple times a day and strictly counting your carbs, etc. I decided if it was in my power to prevent it, I would. Things will get easier for you and your husband, and you’re doing a great job at building a strong support system for yourself, your husband, and your kids.
Thank you! Yes…he’s definitely getting more comfortable swapping sides like rice for an extra veggie. Most restaurants are so helpful!
omg I just experienced almost that same situation beginning of this month ..may 2023
could you please email me
Hugs to you! You two are lucky to have each other, and he’s extremely lucky to have you as his support. I’m confident you guys will knock it out of the ballpark and kick some major booty. Positive thoughts sent to Ohio!
My mom was type 1 diabetic at the age of 10. Before I knew how to spell my name, I knew how to call 911 and how to pour a glass of orange juice for my mom (and where she stashed candy in her purse that was not for me). She was a teacher and I would be the person with her the most. Prayers for ya’ll as you figure out your new normal.
I’m sure our kids will be the same. Thank you!!
I’m 24 and have had Type One since I was 12 and I promise, it gets so much easier! You will all adapt and learn as a family and one day soon all this will feel like second nature.
Continue using social media resources, there is so much great info out there and I would really recommend getting involved with your local JDRF chapter for some support irl.
Lastly I would recommend giving yourselves grace. It’s so easy to feel like everyone else is a perfect diabetic when you see people with perfect A1Cs, running marathons, never going low, etc. but that isn’t reality! We ALL struggle with this disease and have bad days and good days. We all deserve some credit for managing with a life-altering diagnosis and showing up for it 24/7/365 🙂
So true. Thank you so much! We’ll def look into our local chapter.
Thank you Lindsay for sharing your story…I’m sure that it will help so many people who are facing the same things that you and Brett are facing. You are both very strong people and I know that you are up to this life altering challenge. Wishing you all the very best as you undertake this difficult journey. Love to you, Brett and the kids.
Thanks Ron!
My heart is with you. I can identify with the adjustments and with the worry and overwhelm you feel right now. I actually almost cried reading this post because it hit so close to home (I am the mom of a toddler with a recently diagnosed food allergy). It is amazing how many things you do without thought that have to change when things like this arise. Sounds like you guys are doing a great job managing everything so far. Keep up the good work!
Thank you! Thinking of you as well. Food allergies are tough!
Thank you for sharing your story! I wish you and your family all the best with this new life change! I’m curious, does your husband have family history of T1? My granddad has T1 so im thinking I should probably pay attention to any symptoms!
Nope! No history of Type 1 in his family, but I would definitely pay attention in your case!
My husband is Type 1 as well (diagnosed in his early 20s). It might seem overwhelming right now but it will get easier! Having the right medical team will make a world of difference. Good luck to you both on this new path!
thanks so much! we appreciate it.
Love love love that you are sharing and educating!
thanks friend! We’re doing our best.
I was 28 when diagnosed… yep big change and big surprise( no one in the family had ever had type one) but when you get the cgm things will change for the better.
So sorry your hubs has to join the club no one really wants to be part off.
yep! he doesn’t have a family history either. we’re counting the days until a cgm
What an incredible story Lindsay! of bravery and determination, like your life, and a most encouraging attitude. I admire that you’ve seized this opportunity not just to express yourself and share your story – but to help others accept this diagnosis without fear. I’ve followed you since you started, enjoying not just your recipes but also each of your adventures and children’s births. I’m certain I’ll be reading much about DM – and adult onset type 1 is not something I know much about (I specialize in geriatrics). Best of luck and good health.
This post was really interesting. I had a coworker with what he called type 1A diabetes, which he described the same way you describe your husbands type – type 1 onset in his twenties. What I can say is that he got things figured out and it was not all-encompassing the way it is for you now. This season will get easier.
Brett and Lindsay, I’m so sorry to hear you guys are going through this! I can see how it this would feel devastating for a family who spends so much time on health, diet, and fitness. On the other hand, you are informed and well equipped to tackle this disease head-on! Lindsay – if you haven’t found one already, a super awesome and easy website for calculating total carbs in your cooked meals is http://www.sparkpeople.com. You can create recipes, input all the ingredients, and it will spit out all the carb/protein/fat amounts in each serving. Like Myfitnesspal, the website also allows you to keep a daily food ledger where it calculates these same total values. You can save your recipes and later add them with one click when making again or eating leftovers. I used this program when I was vegan for a period of time in my 20s to make sure I was maintaining a healthy protein to carb ratio. I found the user interface really fast and easy to use. Sending you guys many hugs and good vibes!! You can do this!!
thanks Kristin!
It will get easier over time. I’ve had type 1 since 1992. There’s a fantastic T1D community online. Reach out if you have any questions or are feeling like you want to throw your blood sugar monitor at the wall (I may or may not have done this!). You’ve got this!!!
Hello – I know this is almost a year after your original post, but i have never before commented on anything online like this and I just had to say thank you so much for sharing your story. I am 38 and was just diagnosed with LADA about a month ago. For 2 mo before that it was thought to be Type 2. I just really appreciated you sharing your and your husband’s story as i could really relate to the overwhelming amount of information and things to learn and most of all the many questions. Fortunately there seems to be a great diabetes community out there so willing to help and share. Thank you again for sharing and i hope your husband and family have been adjusting to this sudden change well. He has a great supporting partner in you!
good luck on your new journey!
Thank you so much for this read. I am 41 and was just diagnosed type 1 diabetes last week. So much reading and learning to do.
good luck!
Thank our for sharing your family’s story. I am 31 and was just diagnosed with T1 the first week of March. Almost exactly the same symptoms leading up to diagnosis and first week experiences. I appreciate reading your concerns as the spouse as it helps me understand what my husband is worrying about as a Spouse of a T1 diabetic.
Bless you guys!
-Maggie
best of luck to you! it’s overwhelming for sure but it does get easier!
Hello, thank you for sharing your family’s story. My 13yo son was diagnosed with T1D 3 weeks ago, so we are going through the major adjustment. He is doing well considering the shock! We don’t have the CGM or the insulin pump yet, as that takes some time. I was wondering if you found any apps that help with easily getting Carb amount for food, and any apps that you can input your insulin ratio/numbers needed to calculate the bolus and it will quickly calculate the insulin units? It’s easy math, but I would love to find an app that will speed up the process.
Thank you!
i haven’t, but my husband is a numbers nerd so he just does it himself
Thank you for sharing your story. I myself was diagnosed with Type 1 at the age of 29.
I unfortunately,or fortunately however you want to look at it, was well informed/educated in type 1 diabetes and still didn’t look at the signs as seriously as I should have. My son was diagnose in 2012 at the age of one with type 1. You aren’t lying when you say that it is an adjustment for all involved. My son had actually gone in to DKA but like I said, he was one, almost 2, and could not communicate to us what he was feeling. Thankfully we got to the ER in time for them to be able to help us figure out what was going on and starting us on this journey.
Fast forward four years later and I find myself sitting in the ER getting the same diagnosis. Looking back on it the signs were obvious but i put them off as something else every time. I had lost 30 pounds in 2 month, thirsty ALL of the time and urinating frequently among other things. One morning I decided that I would check my blood sugar to rule it out. Sure enough my fasting Bg level was over 500. So to the ER we went
Anyway just wanted to let you know yall are not alone as I am sure you know. The diabetic community is amazingly supportive.
I also noticed you reading the sugar surfing book in one of the pictures. My son’s Endo is Dr. Stephen Ponder. He is amazing !!! the dexcom has changed our lives and I am positive we would not be able to manage our Bg as well as we are able to with out it and the sugar surfing principles
My 20 year old son who is away at college was just diagnosed. Came across this and wanted to say thank you for putting this up. I’m scared, he’s scared but we’ll figure it all out. He has a year and a half left until he graduates so I’ll be a nervous nelly!
Thank you for sharing. I am 30 years old and was just diagnosed on Sunday. I had to go to the ER and spent 3 nights there. This whole thing has been so overwhelming to me and my partner so it is so reassuring to hear your story and know I’m not alone in receiving this diagnosis so late in life.
Thank you for sharing this, my daughter was just diagnosed with type 1 diabetes, how did she find out at the age of 26? She went into Diabetic Ketoacidosis. Her blood sugar was over 500 and blood pressure was at cardiac arrest level, her potassium dropped so low she couldn’t get a breath in. The ICU unit sedated her and had to shock her heart cause it had an irregular heart beat due to her potassium dropping so low, she was intubated and put on a ventilator until they could get her stable. It was beyond scary. Since this happened just last week, she’s still in the hospital in a regular room and doing better, we hope she will go home soon, but then what? What happens now is a huge unknown, she doesn’t have health insurance, so there’s that. Diabetes is by no means a cheap disease.
I would love to know more about any resources you or anyone reading may know about to get supplies cheap, a CGM would be great but I know those are expensive. Any information would be helpful.
Again, thank you for sharing.
Hi Lindsay! Thank you for sharing your familys’ story, gives me hope. Just yesterday I had to go to the ER for possible ketoacidosis… my A1C was at 12.3 and my sugars were in the 300s! Scary. Just about gave my entire family a heart attack.
Thank you for sharing! I’m also 33 and just diagnosed with type 1. I have a very similar story, except I told my mom what was going on and she checked my sugar and it was 530 so I went into the er. And they didn’t keep me so I was in and out for a week! I have the dexcom meter which I love! And trying to get my sugars regulated. They’ve only been normal once so far. But I’m seeing the diabetes educator soon and we can get on a more solid regimen. I’ve always tried to be so healthy and it really sucks to then get type 1.. thanks again for sharing!
Thanks, I’m glad I found your post. I’m an RDN too- but haven’t worked in diabetes for a long time. My 29 yo son was just diagnosed with T1 and like most of the commenters above, we never expected this and are stunned. I’m wondering how people navigate their insurance to get the best coverage, insulin, education, etc. possible. Thanks and blessings to all.